Effective Rehab Boosts Joint-replacement Outcomes
The Next Step
By Mark Morris

Jack Jury says today’s joint-replacement patients experience less pain and a shorter rehab than in the past.
As we age, it’s not unusual for our joints to become worn down from decades of use. For most people, their knees, hips, or shoulders will develop painful arthritis and need some kind of attention.
When a patient suffers from especially severe joint pain, doctors usually begin treatment by recommending physical therapy, as well as pain medications or an assistive device such as a cane or a walker. When these non-operative approaches work, they can provide relief and delay an eventual surgery.
However, “if the pain, function, and quality of life do not improve for the patient, that’s when we recommend joint-replacement surgery,” said Dr. Ben Snyder, an orthopedic surgeon at Cooley Dickinson Health Care.
Nearly 1 million Americans undergo joint-replacement surgery every year, with around 600,000 for knees and 300,000 for hips. According to Snyder, this safe and effective surgery is proliferating because, as people age, they want to remain active through their later years.
In the past, surgeries were often held off until patients were in their 70s because older-model replacement joints would not hold up for more than 10 or 15 years. “But improvements in joint-replacement techniques and technology have increased the longevity of joint-replacement surgery,” Snyder said. “Because of that, we’ve seen a big increase in patients who are 55 to 65 years old.”
A key to success for joint-replacement surgery involves getting patients out of bed and walking on the same day of surgery, Snyder noted. “We find that mobilizing patients early promotes faster recovery, less pain, and fewer complications.”
Andrea Noel-Doubleday, assistant director of Rehabilitation Services at Cooley Dickinson, has been a physical therapist for 25 years. In that time, she said, helping patients with their rehab has improved greatly because it has become a much less painful process for the patient.
Dr. Ben Snyder
“We find that mobilizing patients early promotes faster recovery, less pain, and fewer complications.”
“Joint-replacement surgeries have evolved and become so good that we just guide patients through their exercises,” she said. “For most patients, there isn’t the high level of pain in a rehab like there used to be.”
Less pain also translates to a shorter rehab process. Jack Jury, lead physical therapist at the Rehabilitation Hospital at Mercy Medical Center, said a full knee replacement for many patients is a day-stay surgery.
“They come in in the morning, have their knee replaced, work with us for couple sessions of physical therapy, and then go home the same day,” he explained.
While home exercises and outpatient rehabilitation remain essential, he noted, even they are taking less time. “A few years ago, it was not unusual for our patients to see us for 12 weeks of outpatient therapy. Now, four to five weeks is a long time to work with someone.”
Transition Game
Both Jury and Noel-Doubleday pointed out that rehabilitation hospitals play a key role in the healing process for patients who are not yet ready to move from the hospital directly to their home.
Those patients see people like Nick Rizas, inpatient therapy manager with Encompass Health Rehabilitation Hospital of Western Massachusetts. Rizas explained that patients are usually referred to Encompass because they have chronic conditions (such as obesity, diabetes, and active tobacco use) that make healing more challenging. He also works with patients when they decide to have both knees replaced at the same time.
“When a person is in pain because their knees are giving them trouble, getting both done means they only have to go through the process once,” he said, quickly adding that “this procedure would only happen after a discussion with the surgeon to determine that this is the best course of action.”

Andrea Noel-Doubleday speaks with a joint-replacement patient.
On occasion, physical therapy plays a role before surgery when doctors recommend patients for a program known as ‘prehab.’ Noel-Doubleday explained that prehab allows patients to increase their strength and become familiar with the exercises they will need to perform to properly heal after surgery.
“It can be hard to go through the exercises when you aren’t feeling great, but it’s worth it,” she said. “By being stronger before the surgery, patients can get back to their normal activity sooner.”
When Rizas does prehab work to help patients build strength in their leg or hip before surgery, he said, “it gives them a running head start on their rehab program.”
Healthy muscles around the joint play an important role in protecting it as well, he added, noting that the hips have a deep socket with lots of muscle surrounding them, while the shoulders have less muscle mass protecting them.
“By being stronger before the surgery, patients can get back to their normal activity sooner.”
“The shoulder socket is more like a golf ball on a tee; it’s much more delicate,” Rizas said. “We have to be more careful when treating a shoulder because the muscles surrounding it aren’t as big as in the hips and legs.”
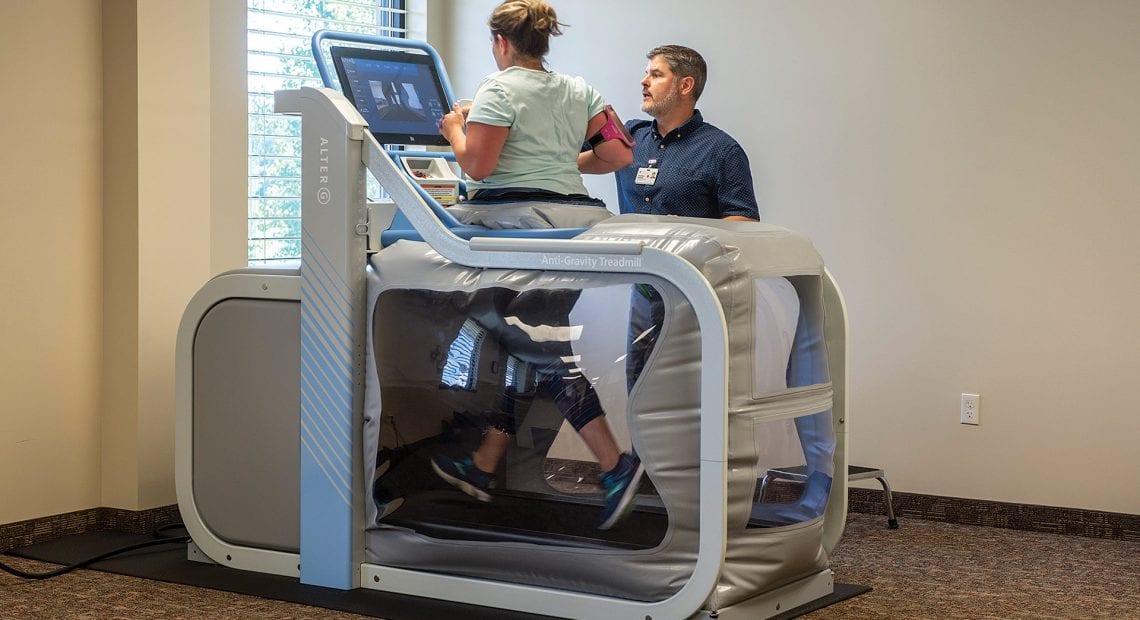
If a patient needs prehab but has trouble walking, therapists now have the AlterG, an anti-gravity treadmill that supports a person’s weight so they can exercise and build their strength prior to surgery. Noel-Doubleday said the treadmill also helps after surgery.
“If a patient is having difficulty getting their normal walking pattern back, the anti-gravity treadmill helps them get more comfortable and confident with their walking and with their movements before their full body weight is on the joint,” she explained, noting that equipment like this was not available even 10 years ago.
Playing Catch-up
One year ago, when COVID-19 infection rates began to overwhelm hospitals, joint replacements, along with other elective surgeries, came to a halt. Elective surgeries have since resumed, and doctors continue to catch up with what Snyder described as “innumerable joint-replacement surgeries” that were put on hold due to the pandemic.
One sign that joint-replacement procedures are back in business, Jury noted, was the recent addition of two new orthopedic surgeons at Mercy Medical Center.
The joint-replacement rehab areas have all beefed up their screening process as well as implemented all the necessary safety protocols to continue to see patients, Noel-Doubleday said. “COVID changed our routine, but it hasn’t stopped us from doing our jobs. We might work with patients in a different space or alter things slightly, but overall, we’ve made the necessary adjustments.”
As the world starts to emerge from pandemic times, many people are concerned about the “COVID 15,” a popular expression for the weight gained as a result of less activity during a year of being stuck inside. Maintaining a proper weight provides many health benefits, and lessening the wear and tear on the joints is one of them. Physical therapists say it’s a simple matter of biomechanics: the more weight we carry, the more stress we put on our joints.
Snyder recently authored a whitepaper on treating knee arthritis and discussed the relationship between weight and our joints. In the data he cited, for every pound a person loses, the force on the knees is reduced by five to 10 pounds.
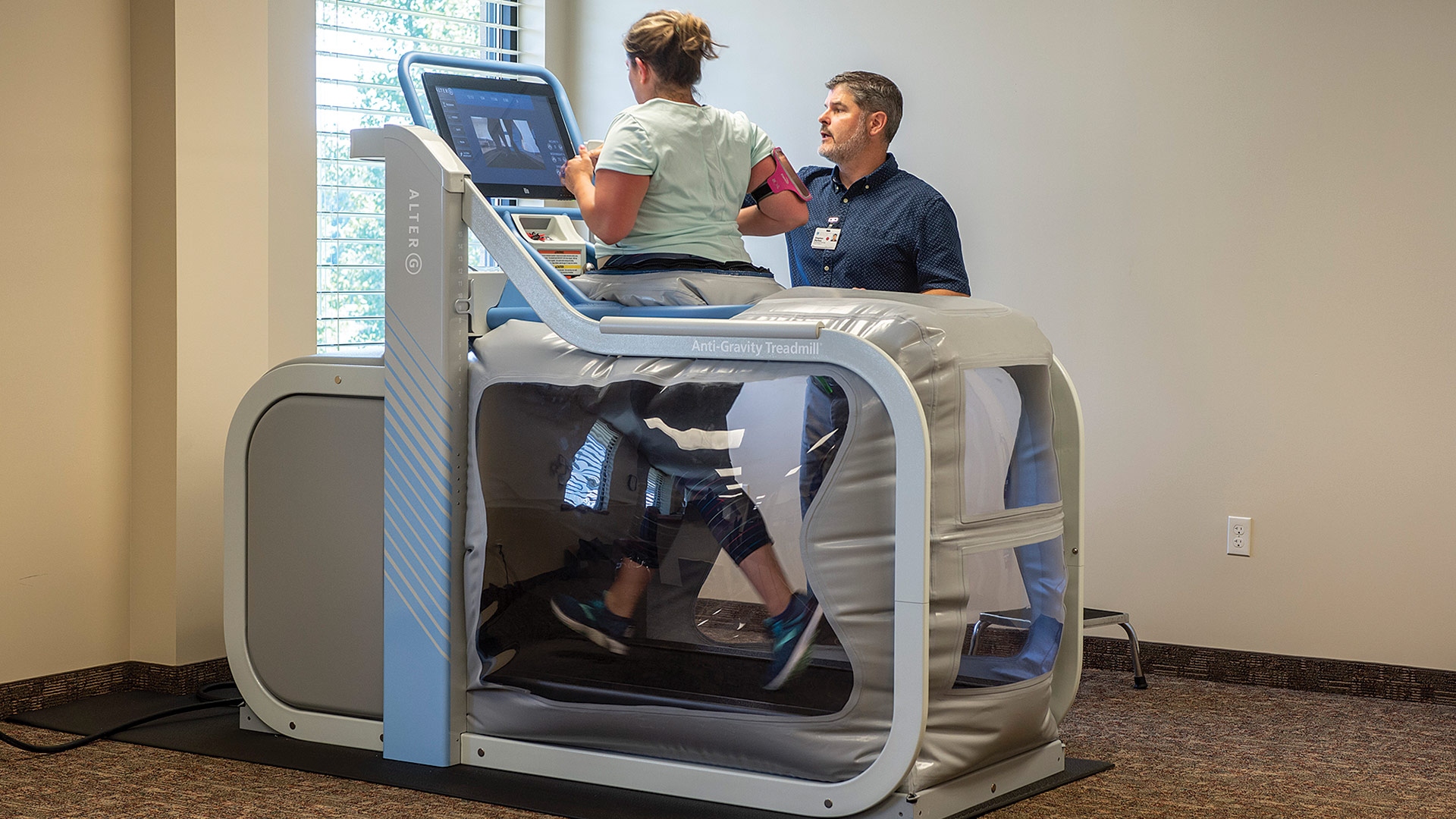
Physical therapist Steve Markey works with a patient on the AlterG anti-gravity treadmill.
Jury said carrying too much weight over time can also throw off structural alignments in the body, which exacerbates the stress on the joints. “We haven’t yet seen the impact from recent weight gains during COVID, and it will probably be years from now until we do.”
When joint-replacement surgery is necessary, Noel-Doubleday makes it a goal to educate patients before the procedure so they know what is involved. Jury makes sure his patients understand what he termed as “a couple important things” to know about joint replacement.
“First, it’s not an easy rehab, by any means,” he said. “But if the patient puts in the effort at physical-therapy appointments and, more importantly, at home with their independent program, they will most likely have a successful outcome.”
He noted that the success rate based on standard outcomes is much better today than it was even five years ago. In turn, most joint-replacement rehab patients these days expect to resume their activities at high levels after surgery. “If you look at walking, the goal is more than comfortably getting around, it’s being able to take a three-mile walk for exercise every day like they’ve done in the past.”
Noel-Doubleday said identifying specific activities patients want to return to is a change from past rehabilitation practices.
“For example, many patients want to resume playing golf or tennis, so we structure the rehab to help them do that again,” she said. “It’s been interesting to see how rehab has evolved like this, and it’s a lot of fun to be a part of it.”





