Before the Fall

Early in Kate Clayton-Jones’s nursing career, she was struck by the cost — both financial and personal — of neglecting preventive care.
Specifically, of the feet.
“I kept seeing a whole bunch of people getting their feet amputated or having surgeries for having fallen,” she said, “and I thought, ‘my God, this is just so preventable.’”
That thought eventually (after plenty of planning, training, and persistence) became FootCare by Nurses, a model for preventive foot care that meets clients — mostly older people — where they are, especially in their homes.
“This isn’t nursing care like, ‘let me come in every day and feed you, clothe you, whatever else,’ but nursing care that could come episodically, once a month, or once every other month, and do this much-needed work, which is taking care of the feet of older adults.”
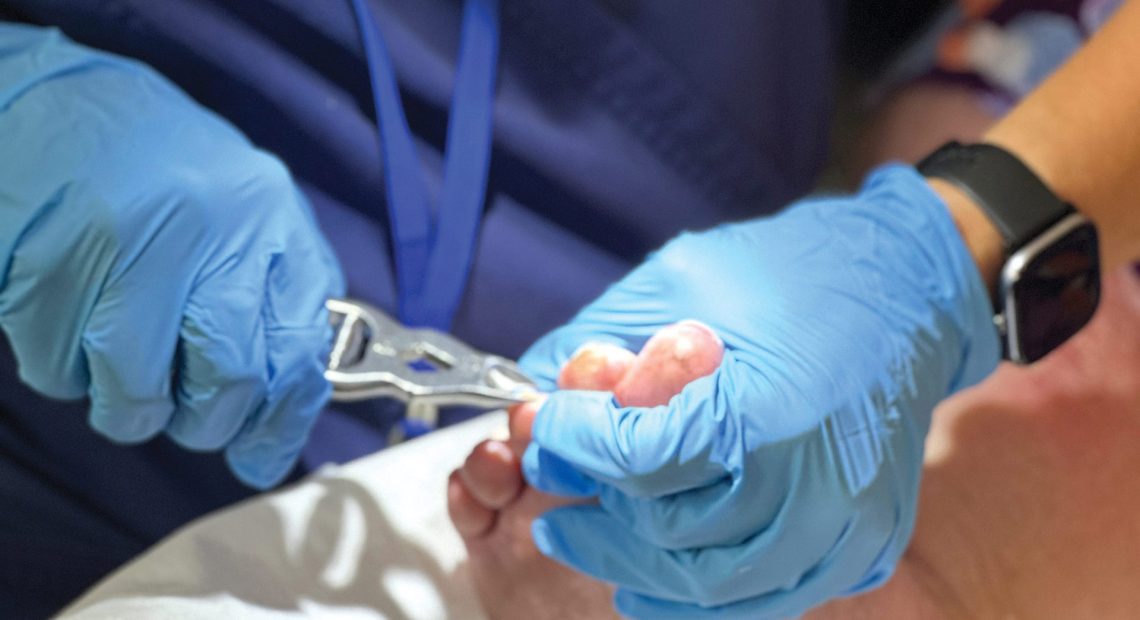
She explained that her nurses sit on the floor and look for circulation problems, sores, and calluses, and release tension in the toes that can limit flexibility and lead to falls. They also check the fit and lacing of shoes and make recommendations about socks. “All our work is designed to improve quality of life. This is an alternative pathway for foot care from typical podiatry or nail salons that most people know.”
For those who would prefer a clinic to a home visit, FootCare by Nurses also has offices in Greenfield, Lenox, and Fitchburg.
“It can be as simple as showing someone how to lace their shoes. We have an opportunity to spend time with people to help them understand simple changes like the way their shoes and socks fit, and skin care. We do a lot with balance and trip hazards,” Clayton-Jones explained.
“Elders are getting touched, and they’re having meaningful conversations. The work we do restores dignity and quality of life. Because we come in as nurses, we can talk about other things as well, and we see them on a regular basis, not just when they have an acute incident.”
While podiatrists are medical doctors whose responsibility is to diagnose and fix problems — recommending treatments and performing procedures — she and her team are licensed nurses with extensive training in foot care, whose responsibility is to prevent problems from happening in the first place. And there is some overlap.
“We have many podiatrists who support this work, though podiatry is a medical intervention, and a lot of this is not medical; it’s basic activities of daily living, and nursing is ideally suited to take care of people in that way,” she said. “There was this gap, and a huge opportunity to do something that is so meaningful, and it’s just a delight.”
The work is important, Clayton-Jones said, because people can become embarrassed by neglected feet and neglect them further — often with dangerous and even tragic results. She was thanked recently by a man whose edema was diagnosed by FootCare by Nurses, and he got the treatment he needed before the situation grew dire.
But even beyond such critical interventions, she said, people are happy when they can simply find pain relief and be able to leave their house or walk with their loved ones.
“We support quality of life in so many ways,” she said. “We not only make a difference when we walk in, but we give them peace of mind. It’s the only type of nursing I’ve done where I’ve heard someone say, ‘I can’t wait for that nurse to come back.’ It’s just such a nice intervention.”
Finding Her Footing
Clayton-Jones didn’t start off as a nurse; in fact, she earned a business degree and was working in aviation before shifting her flight plan to nursing school.
About a decade ago, while working on various floors of Berkshire Medical Center, she encountered patients with inflamed, infected feet, or — even worse — who had broken a hip in a fall, where poor foot care had been a factor. So she asked herself, “why can’t we, as nurses, take care of feet? I can learn to do it.”
So she sought further education through the Wound, Ostomy, and Continence Nurses Society. During that time, she recalls watching a toe amputation of a Korean War veteran who had developed an infection due to ill-fitting shoes a doctor had recommended.

Kate Clayton-Jones at the American Foot Care Nurses Assoc. 2023 National Conference.
“The surgeon did a beautiful job. He was very nice and kind and connected to this man. But the man was very angry because he was losing a part of his body.”
It occurred to her that no one had checked on him and his new shoes — a simple intervention perfect for a nurse’s assessment skills. And she wondered how many other serious infections, debilitating falls, and amputations could be avoided altogether with simple, home-based foot care … by nurses.
After becoming a certified foot-care nurse, Clayton-Jones started treating people’s feet in various setttings. When met with skepticism by people who suggested clients just visit a nail salon, she had a ready answer.
“I said, ‘you don’t understand this population. They’re not able to go out. You’ll never see these people; they’ll never be on your radar, but they are costing the healthcare system an inordinate amount of money when they fall.’”
More importantly, “it gave me great joy to bring dignity and function to these humans who have put so much back into the community,” she added. “These are really incredible people. It doesn’t matter how wealthy or poor you are or where you live — your feet still need to be taken care of.”
By 2016, she had become very busy and realized she couldn’t provide all the care on her own.
“I knew, if I’m going to take on the responsibility of taking care of all these people, this needs to be a real business, with people who want to do this work,” she told BusinessWest. “I will train these nurses, but it needs to be a business that solidly sits on its own foundation.”
In doing so — the business has expanded from three employees in 2016 to 42 today — Clayton-Jones said she’s not only taking care of the community, but providing good jobs for nurses on schedules that work for them, which is especially important if they have families.
“They can start a quarter after nine, after they drop off the kids, see six or seven people, and pick the kid up by three o’clock,” she said, adding that “foot care is not an emergency — it’s prevention.” So if a snowstorm strikes, appointments can be easily moved to a different day. In short, she’s providing nursing jobs with predictable, and not burdensome, schedules.

At right, a nurse at FootCare by Nurses teaches three new nurses how to touch and treat feet.
“I wanted to give them autonomy and responsibility and quality of life while also a joyful, meaningful job that’s not just about trimming toenails, but restoring the best function to an older foot.
“It turns out feet are really, really important,” she added, noting that 40% of cardiac flow is related to foot and leg movement, and toes are part of the body’s ‘seeing’ system for positioning itself in space, so the healthier the feet and toes are, the less likely an older person will fall.
“It’s just preventable with good foot care, good foot function, knowledge about how shoes fit. I started pulling the pieces together — what was behind everything we were doing. And we keep evolving the science.”
And as age demographics in the U.S. keep trending older, it’s a growing problem, especially among the Baby Boom generation.
“They need help — not just care at a podiatry office or a nail salon; they’re going to need this help at home because many can’t drive, or they’re cognitively impaired, or frail. They need to stay home and have care come to them,” she explained. “So the business model was not working with one visiting nurse association or one long-term-care facility — we would work with many, and I would work regionally.”
Next Steps
And the practice is still growing. Clayton-Jones — who regularly speaks on foot-care issues nationally and around the world — recently announced that three new contracts will allow FootCare by Nurses to expand its services in Central Mass., the city of Springfield, and some towns in Connecticut.
A contract with the Program of All-Inclusive Care (PACE) in Springfield will allow Serenity Care case workers to refer clients to FootCare by Nurses. The PACE program is centered on the core belief that, given a choice, most elders, the disabled, and their families would choose to receive care in their homes and communities rather than in a nursing home — so it meshes well with Clayton-Jones’s own mission.
Meanwhile, a contract with Tri Valley Elder Services will expand FootCare by Nurses’ services into the area south of Worcester. Additionally, FootCare by Nurses will take on former clients of Connecticut-based Pedi-care.
“This expansion and continued growth means adding close to 1,000 new clients and $300,000 in new revenue, which will trickle in slowly as referrals for foot care come in,” she said, adding that she plans to add two administrative positions and 10 nursing positions — and is actively hiring for them.
“At the end of the day, if you want a meaningful nursing career, this is just an excellent place. If you’re community-minded, if you like one-on-one conversations where you can make a huge difference, this is really a good career,” she said. “My nurses speak of it as the most joyous job they’ve ever had. They thank me for the autonomy and responsibility, and they get to use all their nursing skills. And they feel connected to the community that they live in, supporting other people.”
As the company grows, its mission — to redefine elder care by making evidence-based foot care central to general health — will not change, she added.
“Our mission is prevention, and our passion is caring. Feet are literally the foundation for our body; they allow us to be mobile, they pump blood back to our hearts, and they connect us to the world. Any fault in feet affects the whole body, just like faults in a foundation affect the entire structure. Yet, feet are too often ignored or neglected, while their care and well-being are essential.”
In short, Clayton-Jones stressed, FootCare by Nurses is not an aesthetic service that simply makes feet and toes more presentable.
“These people need nursing care; it’s a nationwide problem. I can’t tell you how many times I’ve seen nail polish glossing over toenail fungus or a callus or corn, and it continues to perpetuate because no one’s done preventive education,” she said.
“Nurses are educators. We teach people how to take their medications, what the side effects are … a lot of people recognize we’re the healthcare teachers out there. Our mission is prevention. Yes, we’re great at taking care of toenails, but we’re also there to prevent falls or wounds from happening — and we save lives.”